Fetal Therapy
November 16, 2022
PUVs-Posterior Urethral Valves
November 17, 2022
Fetal Therapy
November 16, 2022
PUVs-Posterior Urethral Valves
November 17, 2022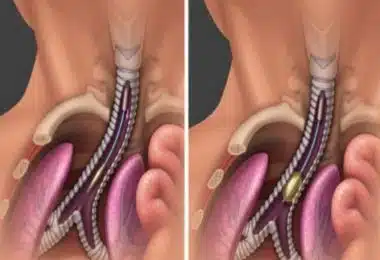
Congenital Diaphragmatic Hernia - CDH
A congenital diaphragmatic hernia (CDH) is a malformation of the diaphragm (a strong dividing membrane located between the abdominal cavity and the chest) that leads to its rupture. As a result of this rupture (caused by a deviation during the development of the diaphragm), organs such as the intestines, stomach, and lungs, which should be located in the abdominal cavity, are displaced into the chest cavity. All this impact on the chest leads to both abnormalities in the development of the lungs and heart failure, making it difficult for blood to flow to the heart and its further pumping to the organs. Lung failure and its related problems, and ultimately death are, unfortunately, the fate of most of the infants born with a diaphragmatic hernia.
A diaphragmatic hernia is a disease that usually occurs accidentally, the genetic inheritance of which is not proven. This rare anomaly occurs once in every 2,000 to 5,000 births.
How Is A Diaphragmatic Hernia Diagnosed?
The diagnosis of diaphragmatic hernia is usually made by ultrasound during a routine examination of the fetus. To ensure the accuracy of the diagnosis, in addition to ultrasound, in rare cases, magnetic resonance imaging (MRI) may be required. Due to the fact that diaphragmatic hernia is often accompanied by chromosomal and structural abnormalities, it is always advisable to conduct an examination for the presence of these abnormalities when planning treatment.
Can Congenital Diaphragmatic Hernia Be Treated in The Womb?
Congenital diaphragmatic hernia varies depending on the type and severity of the disease and carries a risk of death both during surgery in the womb and after birth (due to underdevelopment of the lungs). Not in all cases of CDH, but in those with a particularly poor prognosis (the ones that involve serious risks of lung failure), operations in the womb can be of great benefit. The goal of modern surgical interventions in the womb is to prevent adverse effects on the development of fetal lungs. Nowadays, the treatment method involves the placement of a balloon device in the trachea to ensure that the organs passing from the abdominal cavity to the chest are more resistant to the effect of compression.

Image-1: Fetoscopic endoluminal tracheal occlusion of congenital diaphragmatic hernia with a schematic image of the balloon device (taken from the publications of Texas Children's Hospital).
This procedure (Fetoscopic Endoluminal Tracheal Occlusion) is performed by inserting a camera (fetoscope) into the infant’s respiratory tract, placing a balloon device, and inflating it. There is scientific evidence that this practice can be useful for patients with a poor prognosis. Although small, but there is scientific data on the benefits of steroids and some other drugs in cases of CDH. Thorough research on the treatment of this disease in the womb (with studies on animals and humans) continues.

